Irritable bowel syndrome (IBS): causes, symptoms, diagnosis and treatment
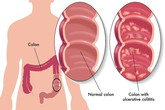
Irritable bowel syndrome is a common disorder that affects the large intestine (colon) and is also known as irritable or spastic colon. It is a functional disorder affecting the functions of the gastrointestinal tract without any abnormality of the structure.
Gastrointestinal system comprises of a tract that starts from the mouth and end at the anus (an opening through which stool passes out) following stomach, small and large intestine. This tract starts working when one takes food; it breaks this food into small particles (digestion) and releases waste products through the anus. IBS does not cause inflammation and can be managed by changes in lifestyle, diet and stress management. IBS is diagnosed when one complains of abdominal pain, cramping, bloating, abdominal discomfort, diarrhea and constipation at least three times a month for the last three months. The symptoms of IBS come and go in episodes, mostly occurring in times of stress or after taking some spicy foods. IBS affects 15% of the general population. It appears that in IBS colon becomes sensitive that is easily upset. This disease is more common in females.
Causes
he exact causes of irritable bowel syndrome are not well understood. It is believed that IBS can occur because of physical and mental problems. Possible causes can be:
Gastrointestinal motor problems
Our intestines are lined with walls. These walls comprise of layers of muscles. The muscles contract and relax in a rhythmically coordinated fashion and push food from the stomach to the intestine and from the intestine to the rectum (terminal part of the large intestine). In IBS, muscle contractions are forceful and prolonged forcing food to move through the intestines readily. It leads to diarrhea, bloating and gas formation. This is not always true for IBS as opposite can also occur in which food moves slowly because of slow muscular contractions leading to hard and dry stools and constipation.
Brain gut signal problems
Brain controls working of intestines by sending signals. These signals travel through nerves and are delivered to the intestines by the nerves of the small and large intestine. Any problem with the brain-gut signals can cause changes in bowel habits, pain and discomfort ultimately leading to irritable bowel syndrome.
Increased sensitivity
The nerves in the gut may become extra sensitive and send more signals to the brain. These sensitive nerves cause the feeling of pain and discomfort in the gut when it is full. Due to this oversensitivity mild indigestion that is rarely perceptible in normal people can cause severe distressing pain in these patients. Increased signal to brain makes one feel hungry or full, or causes urgency to defecate.
Infections
It is proved through a research that IBS occurs after active infection. Those people, who had gastroenteritis - an infection of the gastrointestinal tract caused by the bacteria, develop IBS frequently. Some protozoan infections can also cause IBS. This type of IBS is best treated with antibiotics.
Small intestinal bacterial overgrowth
Small intestine contains some bacteria that are present there normally and do not cause harm under normal conditions. An increase in the number of these small intestinal bacteria can occur abnormally. This leads to extra gas production, diarrhea and IBS.
Psychological factors
Intense emotional states like anxiety and stress can also be a cause of IBS as these states trigger release of some chemicals that disturb normal working of the digestive system. Emotional stress can also affect the nerves of the gut in some susceptible persons. IBS can occur due to some psychological problems as well. These problems include depression, panic disorder, and post-traumatic stress disorder. People who have past of physical or sexual abuse are more prone to develop IBS.
Food triggers
Intolerance to some food can cause IBS. Foods containing high amount of carbohydrates, spicy foods, caffeine, chocolates and alcohol triggers the symptoms of IBS in some people. These triggers vary from person to person. The food sensitivity in a person occurs possibly due to poor absorption of foods like lactose and fructose or deficiency of bile salts (secretions which help in the breakdown of fats) in the body. A diet lacking in fiber can aggravate constipation, as seen in IBS.
Hormones
Some hormonal changes may contribute to IBS. Due to this hormonal influence females are more likely to have IBS and signs or symptoms in them worse during menstruations.
Genetics
IBS tends to run in families. Those people who have some family members suffering the digestive problems more commonly develop IBS.
Signs and symptoms of irritable bowel syndrome
Pain and discomfort
Abdominal pain and discomfort is usually the first complain of people having IBS. It can occur in different regions of the abdomen. Pain does not last all the time, it comes and goes. The duration of each episode of pain varies from person to person and even in a same person during every bout. Pain decreases on passing stools or gas. The severity of pain varies greatly and is colicky in nature.
Diarrhea
Symptoms of diarrhea occurring in patients of IBS include:
- Passing stools 3 or times a day.
- Loose or watery stools.
- Mucous in the stools - whitish clear liquid material in the stools
- Foamy stools
- Urgency.
Constipation
Symptoms of constipation predominant IBS include:
- Hard, dry stools
- Pencil thin stools
- Pellet-like stools
- Less than 3 stools in a week
- Feeling of incomplete evacuation
- Small stools
- Straining
Bloating
Bloating, abdominal distension or abdominal swelling, can occur in some patients.
Flatulence
Excessive gas or wind is common in many persons with IBS.
Tenesmus
Some people may have a feeling of incomplete emptying after going to the toilet.
Urgency
Some people with IBS have an urgent need to go to the washroom. In these people a morning rush is common, often occurring during or after breakfast.
Less common symptoms
These include:
- Nausea
- Headache
- Belching
- Decreased or increased appetite
- Backache
- Tiredness
- Heartburn
- Irritable bladder
Diagnosis of irritable bowel syndrome
Complete medical history and physical examination is necessary for diagnosis. Doctor will ask about family, any history of IBS in family members. As drug can also be a cause so drug history is also necessary. Past history is very important in making a diagnosis because there can be a past history of bacterial infections in some patients. Signs and symptoms are principle factors in making diagnosis. There is a special criterion to diagnose irritable bowel syndrome and some other gastrointestinal disorders called as Rome criteria. These criteria are developed for those conditions in which function of the gut is disturbed while the structure is grossly intact.
According to Rome criteria following symptoms must be present in IBS patients:
- Symptoms are present for the last 6 months
- Abdominal blouting 3 times a month for the past 12 months
- Improvement of abdominal pain after gut movements
- Change in bowel habits like diarrhea, constipation or constipation alternating with diarrhea
- Change in consistency of stool
After asking questions to assess the condition, the doctor will make a diagnosis that whether it is IBS or not. There are some dangerous symptoms of IBS that requires additional diagnostic tests. These red-flag conditions include old age, nausea, weight loss, rectal bleeding, incomplete evacuation and diarrhea that awaken one from sleep. Physical examination of the rectum can detect any discharge of blood or fluid through it, if present. Abdominal examination can be helpful in diagnosis and ruling out other GIT disorders that can cause similar symptoms.
Tests
There are several tests that are necessary for making the diagnosis.
Among the tests to rule other conditions or confirm diagnosis are:
Blood tests
Blood test for irritable bowel syndrome include:
- Complete blood count: To rule out tumors and anemia as this is associated with many gut disorders.
- Liver function tests: To rule liver diseases as these can also cause abdominal pain, nausea and vomiting.
- Erythrocyte sedimentation rate (ESR): This test is specifically used to detect inflammation. Value of ESR rises in inflammatory conditions, as there is no inflammation in IBS value of ESR will be normal in these patients.
- Serologic tests for celiac disease: Celiac disease causes signs and symptoms similar to that of IBS so it is necessary to rule out this disease.
Stool test
In this test one analyzes the sample of stool completely. A container is given to the person in which he/she is asked to collect a stool sample, and then this container is closed and handed over to the laboratory for analysis. This stool sample reveals the consistency and color of stool as well as the presence or absence of bacteria and parasites can be detected. Blood, if present, can also be detected.
Lactose intolerance tests
Lactose is an enzyme that aids in the digestion of sugars and dairy products. Absence of this enzyme can produce indigestion problems similar to IBS. So, there is a need to rule this problem before confirming the diagnosis.
X-Ray
X-ray makes images of the inside and helps in diagnosis.
Computerized tomography (CT Scan)
CT-scan produces cross sectional images of the internal organs. It helps to rule tumors of the rectum or gut and other conditions that can involve gut.
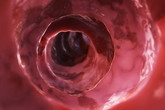
Colonoscopy
Colonoscopy is used for viewing rectum and the entire large intestine. To perform this test patient is given a mild sedative and a painkiller. The patient is asked to lie down and a tube is inserted into the colon through the anus. A small camera is attached to this tube that makes video of inside. Before performing this test patient is advised to take liquid diet 1-3 days before the test and laxative on the evening before the test.
Flexible sigmoidoscopy
Sigmoidoscope is a flexible, lighted tube that aids the examination of the lower part of the colon known as the sigmoid colon.
Endoscopy
In this test endoscope in passed into the gut through the mouth. It helps in ruling out peptic ulcer, inflammatory bowel disease and malignancies.
Hydrogen breath test
This test detects fructose and lactose intolerance and help to differentiate this condition from the others.
Treatment
There is no specific cure for IBS and symptomatic treatment is given to the patients.
Non medical measures
Dietary modifications
The diet that can trigger IBS should be avoided. Large, heavy meals should be avoided as these can also trigger IBS. Instead, small meals should be taken four or five times a day. Fatty foods, milk products, alcohol, caffeine, cabbage, beans and use of artificial sweeteners should be restricted as these can worsen IBS.
Fiber
Fibers make stool soft and easy to pass, therefore, improving constipation. An adult should consume 21 to 38 grams of fiber per day. Fiber rich foods include cereals, beans, vegetables, fruit and grains.
Other advices
- Drink a lot of water to improve constipation.
- Take low-fat diet as fat is a trigger
- Quit smoking, tobacco and nicotine
- Manage stress by taking help of stress reduction and relaxation techniques.
- Add probiotics to your diet.
Medications
Laxatives
Laxatives increase intestinal motility and movements and makes stool soft. They are very beneficial for constipation associated with IBS patients.
Antispasmodics
These drugs relieve painful abdominal spasm and are helpful for IBS patients with diarrhea.
Discontinue PPIs
Proton pump inhibitors decrease the stomach acid production, giving a chance to intestinal bacteria to overgrow and cause IBS.
Anti-diarrheals
Anti-diarrheals like loperamide can control diarrhea. These drugs relax intestine.
Antidepressants
They help in managing depression in IBS patients.
Antibiotics
Antibiotics are helpful for those people in which IBS occurs due to excessive growth of intestinal bacteria. These drugs reduce bacterial growth.
Serotonin agonists
These drugs improve chronic constipation related to IBS but can cause serious side effects too.
Probiotics
Probiotics are living microorganisms, mostly bacteria, similar to those which are normally present in the gut. These probiotics are available in the form of capsules, tablets, powder and help in improving symptoms of IBS.
Alosetron
It is a nerve receptor antagonist that slows down the intestinal movements and relaxes the colon. It can cause serious complications and should be used with cautions.
Lubiprostone
It is used for adult women and men suffering from IBS with constipation. It increases the secretions of intestinal juices that makes stool soft and easy to pass. Side effects like nausea and diarrhea can occur.
| Written by: | Michal Vilímovský (EN) |
|---|---|
| Education: | Physician |
| Published: | May 6, 2014 at 5:50 PM |
| Next scheduled update: | May 6, 2016 at 5:50 PM |
Related articles
Get more articles like this in your inbox
Sign up for our daily mail and get the best evidence based health, nutrition and beauty articles on the web.





Ache in left arm that you should not ignore
Alkaline water dangers: why you should not drink it
How to Avoid Sleepiness While Studying?
23 Foods That Increase Leptin Sensitivity
Low dopamine (e.g. dopamine deficiency): causes, symptoms, diagnosis and treatment options
Swollen taste buds: the ultimate guide to causes, symptoms and treatment
Thin endometrial lining: causes, symptoms, diagnosis and treatment
Pimples inside nose: the complete guide
Holes in tonsils: definition, symptoms, treatment and prevention
How to deal with an ingrown hair cyst
Allegra vs. Zyrtec vs. Claritin
Allergy to penicillin and alternative antibiotics
How to get rid of phlegm (excessive mucus) in throat? Detailed guide to medical and home remedies, symptoms and causes
What causes stomach ache after meals?
Liver blood test results explained