How doctors diagnose Rheumatoid Arthritis (RA)
The first step in the diagnosis of Rheumatoid Arthritis, like in the diagnosis of any other chronic disease, is taking history during which a doctor establishes a few points. Next to history comes the physical examination which usually results in diagnosis. To confirm the diagnosis, laboratory tests are performed.
History
During history taking, doctor asks patient about the presenting complaint, duration of symptoms, systemic manifestations, joint stiffness and a number of other things, the most significant of which is the family history. The family history of a patient is important in diagnosing Rheumatoid Arthritis because this disease has a genetic predisposition, occurring with increased frequency in first degree relatives and monozygotic twins.The sex of the patient, noted during history taking also has a role in diagnosis since RA occurs two to three times more frequently in women compared to men. Age factor is also important since the onset of RA occurs at the age of 30 to 50 years.
Physical Examination
There are a couple of things that doctors look for during a physical examination that helps in establishing an early diagnosis of RA. They look for
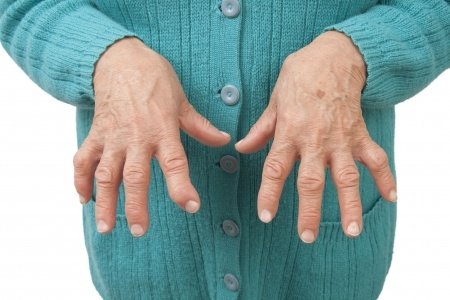
- Bilateral (Symmetric) Swelling of joints of hands, wrists, elbows, knees and ankles for at least six weeks – Bilateral involvement of three or more joints is characteristic of RA.
- Other signs of inflammation such as pain and warmth – RA is an inflammatory disorder so establishing this point further narrows down the diagnosis
- Stiffness (Morning Stiffness) and reduced motion - Morning stiffness refers to stiffness of the affected joints in the morning. This happens as a result of period of immobility at night when the patient is asleep. What happens is that, the joints are inflamed; the inflamed synovial sheath produces excess amount of synovial fluid, projections of synovial membrane protrude into the underlying cartilage and bone causing bone erosions and narrowing of the joint space. Also the inflammation recruits cells to the site. This causes stiffness when the patients wake up in the morning. Because of the same reason, joints show reduced mobility.
- Rheumatoid nodules – these are granulomatous lesions formed as a result of vasculitis in blood vessels of the skin in a subset of patients with RA found over pressure points such as extensor surfaces of the ulna. When present, they are indicative of an aggressive form of the disease. They may resolve spontaneously or they may have to be removed surgically.
Laboratory Tests
The laboratory tests are done to confirm the diagnosis.
Autoantibodies
Normally the immune system produces antibodies against substances foreign to the body and targets them for destruction. In autoimmune diseases such as Rheumatoid Arthritis the immune system starts producing antibodies against self-proteins which causes symptoms of the disease. We call such antibodies produced against self-proteins autoantibodies. As a result, immune complexes are formed which deposit in various parts of the body causing extra-articular symptoms. Doctors can measure levels of such autoantibodies in the blood or synovial fluid to have a clue about the diagnosis.
- Rheumatoid Factor (RF): These are autoantibodies of the type IgM (80% of the time) or IgG produced in approximately 80% of the patients with RA in response to an immunologic trigger which may be environmental such as RA triggering foods (dairy products, meat, etc) so they can be useful in diagnosis when their levels are measured. However approximately 20% of the RA patients do not have RF positive and we call such patients seronegative. Also RF can be positive in a number of other diseases and also in healthy people, so it is not a very specific test. Another deduction that can be made from RF value is that when RF values are very high it means an aggressive form of the disease RA is present and patient should be treated immediately without delay.
- Anti-Cyclic Citrullinated Antibodies (ACCA): Arginine is an amino acid that is a normal component of many proteins in the body. As a result of unusual digestion of arginine in the body, it is converted into an unusual amino acid citrulline. It is believed that when citrulline is incorporated into the body proteins, they become a target for the immune system. Such autoantibodies directed against citrullinated proteins are known as Anti-Cyclic Citrullinated Antibodies (ACCA) and they are very specific for RA.
Radiologic Findings
The X-Rays are an important means to differentiate between RA and other joint diseases but such changes are not present early so they do not help in early diagnosis of the disease. The X-Ray of a late RA patient clearly shows bone erosions characteristic of RA.
Synovial Fluid Analysis
Synovial fluid is a fluid that lubricates moveable joints and reduces friction. Normal synovial fluid is transparent and sterile. If this fluid becomes cloudy and rich in neutrophils, this can be indicative of an inflammatory disorder such as RA. However this procedure can be contraindicated in certain conditions such as cellulitis so doctors don’t always have to use this procedure to make a diagnosis.
Erythrocyte Sedimentation Rate (ESR)
ESR is a blood test that determines at what rate Red Blood Cells (RBCs) settle down. In RA, RBCs settle down at a rate faster than normal, possibly because of additional weight of the immune complexes formed as a result of autoantibodies reacting with the self-antigens. Hence, ESR is increased. This test is not specific since ESR may be increased in a number of other diseases.
C-Reactive Protein
C-Reactive Protein is an acute phase protein produced by the liver into the blood. Its levels are increased in chronic inflammation hence can be measured in the diagnosis of RA. However this test is also not specific.
Complete Blood Count (CBC)
Hepcidin is a protein produced by the liver that is the master regulator of iron. Its levels increase in RA and as a result, iron is no longer available sufficiently for RBC production in the bone marrow.This results in anemia, which can be detected by measuring CBC. This test is also not specific.
Tissue Typing
This is a procedure done just to establish the genetic predisposition to RA.
| Written by: | Michal Vilímovský (EN) |
|---|---|
| Education: | Physician |
| Published: | January 31, 2014 at 1:57 AM |
| Next scheduled update: | January 31, 2016 at 1:57 AM |
Related articles
Get more articles like this in your inbox
Sign up for our daily mail and get the best evidence based health, nutrition and beauty articles on the web.



Ache in left arm that you should not ignore
Alkaline water dangers: why you should not drink it
How to Avoid Sleepiness While Studying?
23 Foods That Increase Leptin Sensitivity
Low dopamine (e.g. dopamine deficiency): causes, symptoms, diagnosis and treatment options
Swollen taste buds: the ultimate guide to causes, symptoms and treatment
Thin endometrial lining: causes, symptoms, diagnosis and treatment
Pimples inside nose: the complete guide
Holes in tonsils: definition, symptoms, treatment and prevention
How to deal with an ingrown hair cyst
Allegra vs. Zyrtec vs. Claritin
Allergy to penicillin and alternative antibiotics
How to get rid of phlegm (excessive mucus) in throat? Detailed guide to medical and home remedies, symptoms and causes
What causes stomach ache after meals?
Liver blood test results explained